One of the most common signs of an aging body is bone loss. It happens to all of us as we get older, but it especially afflicts women for a variety of reasons. The first step to preventing or even reversing bone loss is to understand what causes it.
Understanding Bone Loss Causes
Bones are made of collagen, which is the protein matrix that holds bones together. Most people don’t know this, but there’s a constant cycle of collagen in our bones where it is constructed, destroyed and re-constructed. This is always happening and it’s our body’s way of keeping our collagen healthy.
Osteoporosis occurs when the creation of new bone collagen does not keep pace with the removal of old bone collagen. Throughout our lifespan, bone tissue is constantly being broken down and replaced. When we are young our body makes new bone faster than it breaks down old bone. The opposite is true as we get older, bone mass is lost faster than it is created.
Bone is a living tissue that is in a state of constant turnover. Cells within the bone include:
- Osteoblasts, which are involved in forming new bone collagen; and
- Osteoclasts, which resorb (break down) bone collagen. (When bone is resorbed calcium and other minerals are removed from bone tissue and released into the circulation.)
Both osteoblast and osteoclast activity are needed to maintain healthy bone tissue. The balance between these two opposing activities within bone is influenced by several factors, including:
- Your age
- Your genes
- The number of certain hormones (such as sex hormones estrogen, progesterone and testosterone) in your body
- The amount of physical activity you get (exercise increases osteoblasts to strengthen bones)
- The amount of calcium and vitamin D in your body
- Smoking
- The quality of your diet
The following factors can specifically determine your risk for osteoporosis:
| Too much protein | Too little stomach acid |
| Inappropriate levels of stress | High use of stimulants and fizzy drinks |
| Poor intake of specific nutrients | Poor absorption of specific nutrients |
| Poor use of specific nutrients | High intake of phytates |
| Too much salt | Too much sulfate |
The Symptoms Of Osteoporosis
Osteoporosis does not happen overnight and usually develops slowly without any symptoms over the course of many years. However, a common cause of osteoporosis pain is a spinal compression fracture which can cause:
- Sudden, severe back pain that gets worse when you are standing or walking with some relief when you lie down and becomes chronic over time
- Trouble bending and/or twisting your body, and pain when you do
- Loss of height or “shrinking”
- A curved spine called kyphosis, also known as a “dowager’s hump.”
- Dental pockets
Osteoporosis causes bones to become brittle and weak and therefore easy to break, but it is not a normal part of the aging process – not everyone will get osteoporosis as they get older, despite it being a common occurrence. Some people have a lower bone density than normal because of their habits and genetic markings.
Diagnostic Testing
The bone mineral density (BMD) test is the primary source used to identify osteoporosis and low bone mass. One of the most common ways to measure BMD is by using is dual-energy X-ray absorptiometry or DEXA. This test uses a low-energy X-ray to evaluate bone density in the hip and/or spine and will simply be referred to as a DEXA scan.
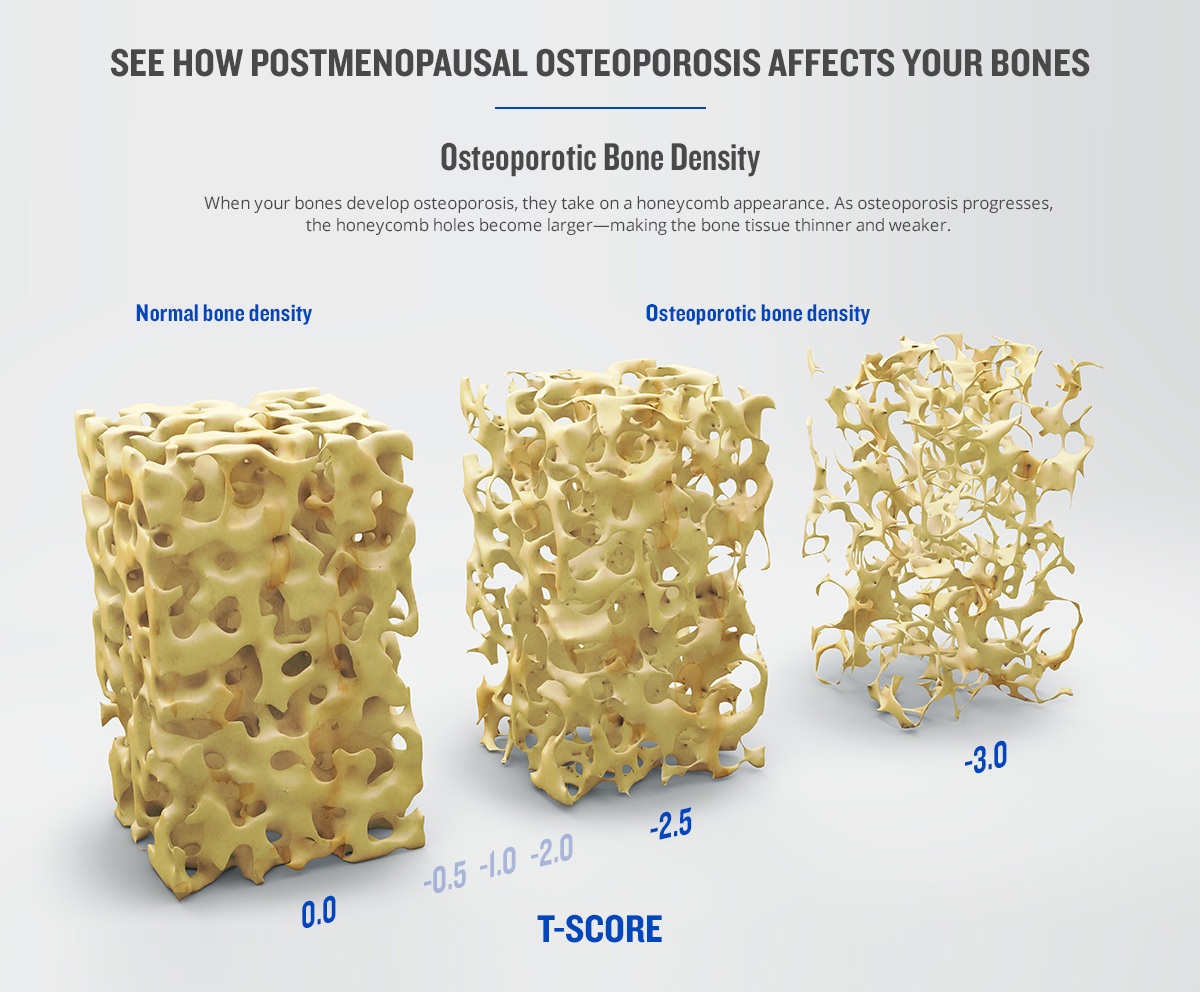
Understanding Your T Score
Your T-score is the measure used when screening for osteoporosis. It is a comparison of a patient’s BMD to that of a healthy 30-year-old that is of the same sex and ethnicity. In post-menopausal women and men over age 50, values for 30-year-olds are used because they better predict risk of future fracture.
According to the World Health Organization:
- Normal is a T-score of −1.0 or higher
- Osteopenia is defined as between −1.0 and −2.5
- Osteoporosis is defined as −2.5 or lower, meaning a bone density that is two and a half standard deviations below the mean of a 30-year-old man/woman
Preventing And Treating Bone Loss Naturally Versus Using Medication
Taking an osteoporosis medication may help decrease the risk of fracture but the possibility of a break is not eliminated completely. The most commonly prescribed medications for bone loss are bisphosphonates such as Fosamax, Actonel, Aredia, and Zometa. These medications have not been found to be a cost-effective way to treat osteopenia and osteoporosis. Most people do not suffer major side effects of the medications but there have been some cases of atypical femur and jaw fractures. There have not been any long-term studies done on the effectiveness of these drugs. They are typically prescribed for a period of three to five years. Some doctors worry that staying on the drug for more than five years can cause some women’s bones to become more brittle and break spontaneously.
These drugs increase the mineral framework of the bones but recent research has shown that the trabeculae (cross bars) of the bone matrix may not be stronger thus making the bones still susceptible to breaking.
The women on these drugs have a false sense of security as they get regular bone density tests. The tests usually show a steady increase in bone density which doesn’t make any sense. Essentially the crossbars are denser but not stronger. This puts them at risk of serious spontaneous fractures.
Calcium Alone Will Not Do It
It is important to understand that osteoporosis is not a calcium deficiency disorder – it is a disorder where calcium is lost from bone. Ninety-nine-percent of calcium in the body is in bone. Just replacing calcium and giving vitamin D that aids calcium being deposited in bone is linear thinking in terms of managing this devastating, largely preventable disease. Up to four-percent bone loss per year can occur by the time a woman reaches her late sixties.
Taking a calcium/magnesium/silica supplement along with a vitamin D3 supplement and Vitamin K2 could help prevent and treat bone loss. Calcium/magnesium/silica as well as zinc build bones and keeps them healthy. Vitamin D helps the body absorb calcium. Vitamin K ensures the calcium gets where you need it – your bones, instead of your organs which could cause a number of health problems including atherosclerosis and kidney stones. Magnesium is vital in creating the spark within the cell to utilize calcium.
Another supplement that could be helpful is hydrolyzed collagen which has been found to help reduce bone loss and restore bone density in postmenopausal women. Collagen helps create the cement which holds the trabeculae. This way the crossbars are denser and stronger.
Collagen peptides (CP) compounds, as bone health supplements, are known to play a role in the treatment of osteoporosis. However, the molecular mechanisms of this process remain unclear. One study aimed to investigate the effects of bovine CP compounds on the proliferation and differentiation of MC3T3-E1 cells. What the study found was that bovine CP compounds increased osteoblast reproduction and played positive roles in osteoblast differentiation and mineralized bone matrix formation. Essentially, the authors concluded that their study indicated taking a bovine CP compound like Collagen Complete could be beneficial for the potential treatment of osteoarthritis and osteoporosis.
Balancing Hormones
A major factor contributing to the onset of osteoporosis in women is the decline in hormone levels after the onset of menopause, as all the major sex hormones play an important role in maintaining bone density. One in four postmenopausal women has osteoporosis. Progesterone is considered the most important hormone as it is able to stimulate osteoblast-mediated new bone.
Prevention Osteoporosis Naturally
The best way to prevent osteoporosis and osteopenia is to stimulate the body’s collagen-creation cycle so that you are making more collagen than you’re destroying.
This can be done through diet, exercise, and outdoors activities. These may also help in slowing down osteoporosis.
The Best Bone Density Exercises
Regular weight-bearing exercise throughout life is best but it is never too late to start.
Walking, running, jumping in place, playing tennis and taking an aerobics class are all weight-bearing exercises that promote healthy bones. Muscle-strengthening exercises include lifting weights, using exercise bands or doing calisthenic exercises. Tai Chi is also very beneficial. It is important to get some kind of exercise every day.
Both weight-bearing and muscle-strengthening exercises will help build and maintain bone density.
The reason weight-bearing exercise is helpful is twofold: 1. It triggers the collagen cycle of destruction and reconstruction that we discussed above, and 2. It stimulates healthy hormonal balance.
Preventing Osteoporosis With Nutrition
Eating a healthy balance of fruits and vegetables is vital. Meat, egg yolks, cheese and fatty fish such as sardines, sockeye salmon, mackerel, herring and tuna are a good source of calcium and Vitamin D, however, sun exposure is still the best source of Vitamin D. A healthy diet is made of healthy fats, wholesome foods and healthy sources of protein.
Other Important Bone Nutrients
| Nutrient | Best Food Sources |
| zinc | nuts, seeds |
| manganese/boron | unprocessed foods |
| silicon/copper | unprocessed foods |
| vitamin A | yellow and deep green vegetables |
| vitamin C | berries, potatoes, most fruit and vegetables |
| vitamin K | cauliflower and green vegetables |
| vitamin B6 | fruits, vegetables |
Hydrolyzed Collagen, Collagen Peptides, And Easy Absorption
As with most diseases, prevention is better than curing an infliction after it is already taken hold of your body. Staying active and eating a healthy, balanced diet is one way to keep bones healthy and prevent excessive bone loss. Getting a daily 20 minutes of sun exposure (not a sunburn) and fresh air is another way to prevent “thinning.” Supplementing with the correct minerals, vitamins and collagen will add to your healthy regimen and contribute to a healthy strong frame. All these can easily become part of your healthy daily living.
As discussed above, using a supplement such as Collagen Complete can help replenish your bones and increase bone density.
Try Collagen Complete